
Beginning January 1st, New Jersey Medicaid implemented new changes to support the health and safety during pregnancy. Learn more via our latest Quality Briefing.
The Medicaid Policy Center (MPC) is dedicated to advancing the quality and cost effectiveness — and long-term sustainability — of the New Jersey Medicaid program to improve the health and wellness of New Jersey residents.
The MPC delivers independent research, analysis and policy solutions to improve health outcomes while also controlling costs — and works in partnership with other organizations and the state government agencies that operate the New Jersey Medicaid program.
The center benefits from the Quality Institute’s tradition of bringing people from all corners of health care together to collaborate on innovative solutions to improve the state’s health care system.
Beginning January 1st, New Jersey Medicaid implemented new changes to support the health and safety during pregnancy. Learn more via our latest Quality Briefing.
The New Jersey Reproductive Health Access Project (NJ-RHAP) is a statewide initiative created to empower New Jersey patients, their providers, and payers, to identify the reproductive health services that are best for themselves and their families and to expand access to the full range of contraceptive options available. NJ-RHAP seeks to identify and improve state laws, regulations, and contracts while increasing providers’ understanding of key policies that impact service delivery for reproductive health services, specifically contraceptive services.
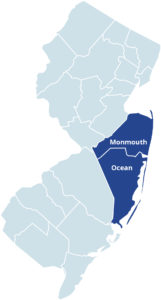
Hackensack Meridian Health (HMH), in partnership with New Jersey Medicaid, New Jersey Health Care Quality Institute and the Visiting Nurse Association of Central Jersey, has entered into a collaborative agreement with Centers for Medicare and Medicaid Services (CMS) to establish the NJ Integrated Care for Kids (InCK) model. Working with those who provide primary care to children in Monmouth and Ocean Counties, NJ InCK will test an Alternative Payment Model (APM), for NJ Family Care programs, by providing payment for screening and provision of integrated community-based core child health services.
Ensure that all children receive expanded EPSDT (Early Periodic Screening, Diagnosis, and Treatment) care at least annually;
Identify children and adolescents who have more complex health, behavioral or social needs; and
Provide community-based care management that integrates with the pediatric health system.
The NJ InCK Model will include: integrated advanced case management, care planning, and community health workers. When gaps in population-based services are identified, NJ InCK will advocate for new clinical modalities. The NJ InCK Model will increase flexibility for selecting treatment modalities for adolescent substance use disorder.
NJ InCK’s APM blends base funding and incentive payments to support eventual implementation of a shared savings APM built on New Jersey’s managed care program. The APM will incentivize higher screening rates to support appropriate patient stratification, connection to needed services, and intensive case management for high-needs children.
In addition to the three co-lead organizations, additional project partners include the New Jersey Chapter of American Academy of Pediatrics and the Central Jersey Family Health Consortium. The project will also engage with a Partnership Council consisting of entities including local health departments, stakeholder representatives, Medicaid managed care organizations, and providers responsible for core child services, including physical and behavioral clinical care, schools, housing authorities, food support services, early care and education, Title VI agencies, child welfare, and mobile crisis response services
NJ-RHAP is a statewide initiative created to empower New Jersey patients, their providers, and payers, to identify the reproductive health services that are best for themselves and their families and to expand access to the full range of contraceptive options available. NJ-RHAP seeks to analyze and improve state laws, regulations, and contracts while increasing providers’ understanding of key policies that impact service delivery for reproductive health services, specifically contraceptive care. The goal of NJ-RHAP is to reduce the policy and payment system barriers that prevent individuals from accessing their preferred birth control methods through provider education efforts and to promote policy change that supports patient-centered reproductive health care.
Works with state and national entities, stakeholders, and subject matter experts to identify barriers patients and their providers face in trying to access various methods of contraception;
Developed a toolkit to provide guidance and clarification on key policies impacting service delivery and reimbursement for reproductive health services, as well as best practices for patient-centered care, and disseminates this information in a variety of formats to providers throughout the state; and
Leverages the expertise of its members, project consultants, and the NJ-RHAP Steering Committee to identify and form recommendations to policy issues regarding accessible reproductive health services.
In Summer 2020, the Quality Institute released the NJ-RHAP PACT, an engaging and informative resource for providers. The NJ-RHAP PACT provides education and support for the implementation of best practices to increase access to reproductive health services, including long-acting reversible contraception (LARC), using shared-decision making and the promotion of reproductive justice. The toolkit covers topics such as billing and coding for contraceptive services, same-day access to LARC, and community engagement strategies.

